
Definition
• It is the process of measuring the temperature, pulse, respiration, blood pressure, and pain of a client/patient to detect any deviations.
Temperature assessment
• This involves measuring the balance between heat production and heat loss by the body.
Pulse assessment
• This is the measurement of pressure pulsation created when the heart contracts and ejects blood into the aorta creating a wave of expansion and recoil in the arteries
This can be felt by palpation at a point where an artery crosses a bone close to the surface.
Pulse oximetry
• This is the measurement of arterial oxygen saturation using non-invasive light.
Respirations assessment:
• This is the measurement of the breathing pattern and rate.
Blood pressure assessment
• This is a measurement of pressure exerted by blood on the walls of its vessels.
Pain assessment
• This is evaluation of reported pain and the factors that alleviate or exacerbate it, as well as response to treatment of pain.
Purpose Of Taking Vital Signs

• To collect data on the body’s response to physical or psychological stress or changes in physiological function to determine a patient’s health status.
Indications Of taking Vital Signs
• Clients/Patients seeking health services
A. Assessment
Assess for;
1. Appropriateness of working environment to determine its ability to provide comfort, privacy, and enhance efficiency.
2. Equipment required to determine equipment availability and functioning status.
3. Client’s/Patient’s physical and mental status to determine assistance required and if the patient can give consent
4. Client’s/Patient’s understanding of the procedures to determine the teaching needs of the client and gain their cooperation, minimize anxiety.
5. Site to be used for measurements to determine suitability as some conditions affecting these sites can interfere with accurate readings.
6. Foods/drinks taken in the last 15-30 minutes to establish if hot or cold foods/drinks have been taken that would influence the accuracy of temperature.
7. Activities performed in the last 15-30 minutes as hyperactivity may increase sympathetic nervous system activity and interfere with the accuracy of data.
8. Presence of skin lesions to institute correct interventions.
Planning (taking vital signs)

Preparation of Self
• Hand hygiene
• Review procedure
• Review factors that influence vital signs
Preparing The Patient
1. Explain the procedures to the patient and obtain consent.
2. Ask the client/patient if he/she has taken hot or very cold drinks/food within the last 30minutes.
3. Ask the client/patient to rest for at least 5 minutes before the procedure where applicable.
4. Explain to the client/patient that he/she will be required to relax and breathe normally when vital signs are being measured.
Preparing The Environment
• Privacy of the room
• Cleanliness of the room
• Adequacy of lighting and ventilation
• Availability of standard operating procedures
• Adequate working space
Requirements For Taking Vital Signs
A clean trolley with;
Top shelf;
A clean tray containing;
• A thermometer (as per institutional policy)
• A pack of clean and dry cotton wool balls
• A gallipot
• Surgical spirit /antiseptic solution
• Lubricant (for rectal temperature)
• A watch with a second hand
• Pulse Oximeter
• Sphygmomanometer and Stethoscope
• Clean gloves where necessary
Observation charts/pain assessment chart
Paper to record findings for reporting
Bottom shelf;
• Decontaminant in a container
• A receiver for used cotton wool swabs
Implementation (Steps) in vital signs
How To Take Temperatures
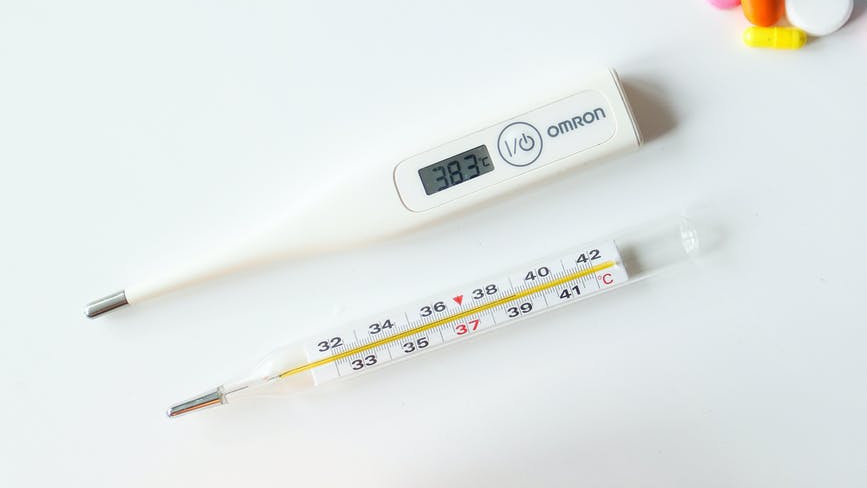
1. Take the equipment to the bedside/next to the patient for ease of accessibility.
2. Identify the patient to ensure the right procedure for the right patient.
3. Explain procedure to the patient to allay anxiety and gain co-operation
4. Wash and dry hands for infection prevention and control
Axillary and groin
5. Dry axilla/groin with a clean cotton wool Swab to ensure sweat and moisture do not interfere with the reading of the thermometer
6. Place a thermometer in the axilla/groin making sure that the thermometer bulb is fully covered by the skin folds.
This allows for close contact of the bulb with the superficial blood vessels for accurate temperature registration.
7. Switch on the thermometer and position it while the arm or thigh is held firmly by the patient or nurse to prevent the thermometer from dislodging from the axilla during the procedure
8. Gently remove the thermometer, when it alarms or after 4-7 minutes (for non-digital thermometers) and read.
Thermometer alarm alerts that the reading is complete, and the nurse should read, interpret and record the findings.
4-7 minutes allows for adequate time for contact between the bulb and the superficial blood vessel for accurate temperature recording
Rectal
1. Wash hands and wear gloves for infection prevention and control.
2. Explain the Procedure to allay anxiety and gain cooperation
3. Position child in a left lateral position to promote ease of access and insertion of the thermometer.
4. Lubricate thermometer and insert 1-2 cm depending on the age of the child to prevent injury to the anal and rectal tissues and allow the bulb to be covered by rectal mucosa.
5. Hold the thermometer in position until it alarms while talking to the mother or child.
This prevents dislodging of the thermometer and ensures accuracy of the reading and reduces the child’s/mother’s anxiety through engagement.
6. Gently remove the thermometer, wipe with a clean dry swab from the stem to the bulb using rotating movement, and taking care not to touch the bulb.
This helps reduce the transfer of micro-organisms and tampering with the mercury level.
7. Ensure the child’s buttocks are cleaned and dry to promote the patient’s hygiene and comfort.
NB: For any other thermometer follow the manufacturer’s instructions to ensure accuracy if reading.
How To Take A Pulse

Radial Pulse
1. Flex patient’s elbow and place lower part of the arm across the chest.
Relaxed position of forearm and slight flexion of wrist facilitates accessibility of artery for palpation.
2. Place the tips of the index and middle fingers over the radial artery applying light but firm pressure.
This facilitates palpation since fingertips are sensitive and better able to feel the pulse. Light pressure prevents occlusion of blood flow.
3. N/B: do not use your thumb to palpate the pulse to avoid the feeling of the strong pulse of the thumb
4. Palpate for pulsation and count the pulse rate for a full minute. (Note rate, rhythm and volume).
This helps detect any deviation from normal and plan for appropriate intervention.
5. Record findings on the appropriate chart to communicate findings.
Apical Pulse (Apex Beat)
1. Position patient on left side and expose patient’s sternum and left side of the chest.
This allows access to the patient’s chest for proper placement of stethoscope and selection auscultatory site
2. Palpate for apical pulse. Auscultate for apical pulse over the fifth intercostal space, left of the mid clavicular line and mark the site where you feel it.
This ensures that the point of maximum impulse is identified for accurate measurement.
3. Clean the earpiece and diaphragm of the stethoscope with antiseptic cotton wool swabs for infection prevention and control.
4. Warm the diaphragm of the stethoscope by holding in the palm of your own hands for 5 to 10 seconds to avoid startling the patient and altering pulse rate.
5. Insert earpieces of stethoscope into own ears and place the diaphragm over the fifth intercostal space, left of the mid clavicular line as shown in the figure below.
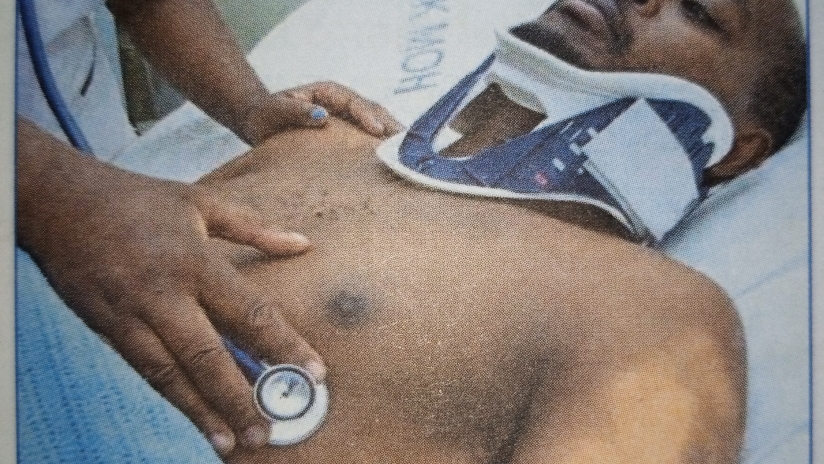
The point of maximal impulse is anatomically located at this position, hence promoting the accuracy of heartbeat measurement.
6. Listen to the beats for rhythm, strength, and rate to detect any irregularities, which may indicate inadequate cardiac perfusion and output.
7. Inform the client/patient when the procedure is over, cover the patient and leave him/her Comfortable to ensure comfort and cooperation.
How To Take Respirations

1. With the fingers still in the pulse position, observe the patient’s chest movements without drawing the patient’s attention to the activity.
This avoids causing alterations in breathing patterns that occur when the client is aware respiration is being assessed.
2. Observe one complete cycle of respirations; count the respirations for one full minute to avoid inaccurate data.
3. Note chest expansion, depth, and rate of respiration. Alterations in rate, depth, and rhythmic chest movements would be an indication of respiratory, renal, and other system anomalies.
4. Record findings to communicate findings and for subsequent comparison of progress.
How To Take Blood Pressure
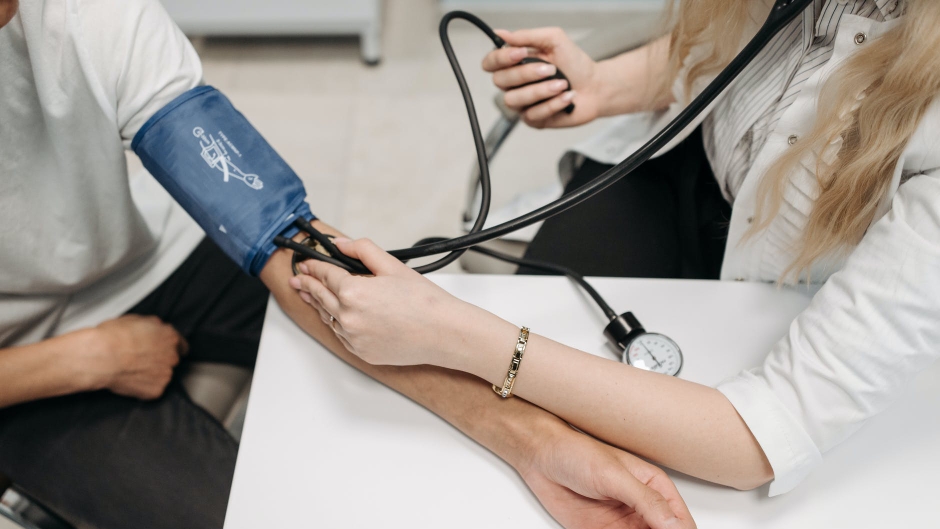
1. Assist client/patient to a comfortable position with forearm supported at heart level and arm duplicated
This ensures an accurate reading. Stress may affect the blood pressure measurement.
2. Expose the upper arm completely and ensure no tight clothing to allow accurate placement of the cuff and stethoscope and ensure the reading is accurate.
3. Place the sphygmomanometer on the bed or locker at the same level as the patient’s heart to ensure accuracy of reading.
4. Deflate the bladder cuff fully and test the pump to ensure it moves freely to confirm the functional status of the machine for the effectiveness of the procedure.
5. Palpate brachial artery in the antecubital space and place the cuff so that the midline of the bladder is over the arterial pulsation.
6. Then wrap the deflated cuff snugly and evenly around the bare upper arm ensuring that its lower edge is 2 cm above the antecubital fossa where the stethoscope head is to be placed to allow for identification of the artery.
For mercury sphygmomanometer, ensure it is vertical and at eye level to prevent distortion and promote the accurate reading of mercury level.
7. With a non-dominant hand, palpate the brachial artery with fingertips, the dominant hand closes the pressure bulb valve and inflates the cuff until the pulse disappears.
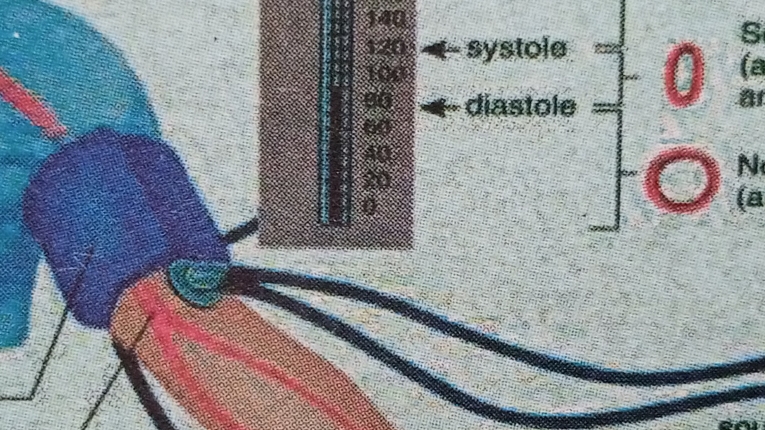
Continue to inflate the cuff 30 mmHg above. Slowly release cuff and while still palpating, note when pulse reappears to prevent air leak.
8. Fully deflatethe cuff and wait for 1-2 Minutes to allow recirculation of blood trapped in the vein.
9. With the dominant hand close the pressure bulb valve, place the stethoscope earpiece in its ears to fit snugly, re-palpate the brachial artery as in step 7 and place the stethoscope bell or diaphragm over brachial artery located site for audibility of the heart sounds.
10. Re-inflate the cuff as in step 7 and slowly release the valve to deflate the cuff at 2 mmHg/sec while listening to identify the 5 phases of korotkoff sounds and the mercury levels at which they appear for an accurate reading.
11. Deflate cuff completely and remove from patient’s arm and assist patient to a comfortable position as appropriate to complete the procedure and release patient for other activities.
12. Clean the earpiece, bell, and diaphragm for infection prevention and control with an appropriate antiseptic.
13. Store equipment Appropriately for safety and in readiness for next use.
14. Record findings, noting Abnormalities for baseline data, comparison, and continuity of care.
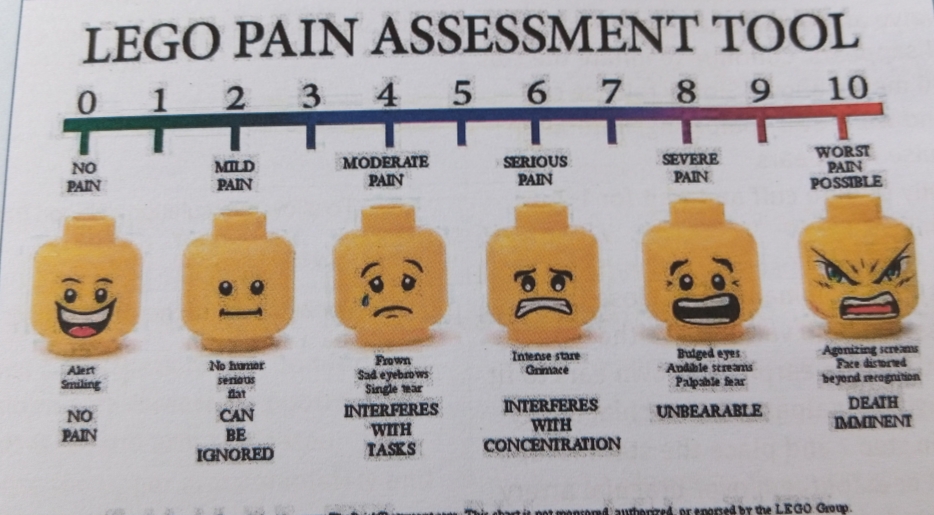
How To Assess For Pain

1. Ask the client/patient if they are in pain and if he/she cannot communicate, use the appropriate nonverbal pain assessment tools to ascertain the presence and level of pain.
2. If they are in pain, use a validated pain assessment tool for correct rating and quantifying of pain.
3. Document findings and take appropriate action to communicate data, and use it to evaluate the effectiveness, of actions taken to relieve pain.
• Evaluate if the vital signs were assessed appropriately and if deviations from normal were noted for completeness, detection with future appropriate comparison, planning, and interventions reading abnormalities.
Always remember to record;
• The date and time procedure was done
• The vital signs: Pulse, Respiration rate, Blood Pressure, Oxygen saturation, Temperature, and pain score on the appropriate chart.
• Time and frequency of measurement
• Action taken
• Patient’s response during the procedures
• Your name and append your signature
Leave a comment